Contraceptives
Contraceptives are ubiquitous, they are being used in the remotest rural areas. But at what cost?
All drug based contraceptives, whether they are a combo oestrogen/progestin or progestin only, can cause many adverse side affects...
- depression
- an increased risk of post natal depression
- follicular cysts
- SHBG capacity decreased
- insulin resistance
- lowered progesterone levels
- an increased risk of breast cancer
- an increased risk for invasive cervical cancer
- DNA damage
- elevates CRP leading to inflammation with a risk of future heart disease
- can cause fatty deposits on the linings of arteries
- raised cholesterol
- causes platelet aggregation leading to blood clots
- increases blood pressure
- potential to exacerbate asthma
Contraceptives and HRT are similar drugs. The ingredients are based on natural or synthetic oestrogen, given alone or in combo with a progestin, a synthetic progesterone. The proportions are slightly different, generally contraceptives contain higher levels of progestins, and HRT contains higher levels of oestrogen. Some examples for comparison are given below...
Contraceptives
|
Mirena IUD Provera tablets Intramuscular injection Yasmin tablets Yaz tablets Beyaz tablets Alesse tablets Apri tablets Brevicon tablets Ovral tablets |
52 milligrams of levonorgestrel 2.5, 5, and 10 mg of medoxyprogesterone acetate (MPA) 150, 160, and 400 mg/ml of MPA 3 mg of drospirenone and 0.03 mg of ethinyl estradiol 3 mg of drospirenone and 0.02 mg of ethinyl estradiol 3 mg drospirenone, 0.02 mg ethinyl estradiol 0.10 mg of levonorgestrel and 0.02 mg of ethinyl estradio 0.15 mg desogestrel and 0.03 mg ethinyl estradiol 0.5 mg norethindrone and 0.035 mg ethinyl estradiol 0.3 mg of norgestrel and 0.03 mg of ethinyl estradiol |
HRT
|
Vivelle-Dot patch CombiPatch Premarin tablets Premarin injection Premarin Vaginal Cream Prempro |
0.025, 0.0375, 0.05, 0.075, or 0.1 mg of estradiol 0.62mg estradiol/2.7mg norethindrone acetate or 0.51mg estradiol/4.8mg norethindrone acetate 0.3 mg, 0.45 mg, 0.625 mg, 0.9 mg, and 1.25 mg of a mixture of conjugated estrogens, sodium estrone sulfate, sodium equilin sulfate, sodium sulfate conjugates, 17Œ±-dihydroequilin, 17Œ±- estradiol, and 17Œ±-dihydroequilin. Blended to represent the average composition of material derived from pregnant mares' urine vial contains 25 mg of conjugated estrogens, also lactose 200 mg, sodium citrate 12.2 mg, and simethicone 0.2 mg. The pH is adjusted with sodium hydroxide or hydrochloric acid. 0.625 mg conjugated estrogens, sodium sulfate conjugates, 17 Œ±-dihydroequilin, 17 Œ±-estradiol, and 17Œ&Mac178;-dihydroequilin. In a nonliquefying base containing cetyl esters wax, cetyl alcohol, white wax, glyceryl monostearate, propylene glycol monostearate, methyl stearate, benzyl alcohol, sodium lauryl sulfate, glycerin, and mineral oil 0.3 mg (as for Premarin)/1.5 mg MPA and 0.45 mg (as for Premarin)/1.5 mg MPA, 0.625 mg (as for Premarin)/2.5 mg MPA, 0.625 mg (as for Premarin)/5 mg MPA |
The only safe contraceptive is the copper T IUD. It leaks no drug into the body, and it's efficacy is similar to drug based contraceptives. A review of several studies showed the copper T IUD to be better at preventing pregnancy than depot medroxyprogesterone acetate (DMPA).
An alternative to the copper T is the GyneFIX. This is also a hormone free, copper based intrauterine device.
Other alternatives are devices that do not contain hormones and create a physical barrier, such as condoms (male and female), or cervix caps.
Many progestin only contraceptives are derived from testosterone, and have androgenic properties. Undesirable side effects associated with this include acne and seborrhea, weight gain, blood pressure increase, an increase in the low-density lipoprotein (LDL) to high-density lipoprotein (HDL) ratio, facial hair, hair loss from the head and aggression.
In addition, they have been shown to have oestrogenic activity too and to stimulate proliferation of breast cancer cells.
The combo oestrogen/progestin can lead to an increase in water retention, weight gain, cancer and more.
Medoxyprogesterone acetate (MPA) is used to facilitate infection of herpes in animal models of sexually transmitted diseases. MPA also functions as a tumour promoter.
Contraceptives can result in temporary infertility after stopping them. They are designed to stop ovulation, but once stopped the ovaries can start up again. Initially making oestrogen and testosterone, it can be many cycles later before ovulation takes place. This initial surge of oestrogen and testosterone causes a severe imbalance in the ovaries and anovulation results.
Luteinising hormone (LH) is secreted by the anterior pituitary gland and is required for both growth of preovulatory follicles and ovulation of the dominant follicle. In an effort to make a mature follicle ovulate the pituitary increases output of LH, but excess LH suppresses ovulation.
LH also stimulates proliferation, differentiation, and secretion of androgens by the theca cells which surround the ovum, hence the rise in androgen levels. This rise is responsible for the acne, oily skin, facial hair etc., that many women find occurs after discontinuing the contraceptive.
With excess androgens, oestrogen also increases. The androgens, notably androstendione, migrate from the theca cells to the granulosa cells where it is converted by the enzyme aromatase into oestrogen, particularly oestradiol. The theca cells also produce oestradiol without the need for conversion. The excess oestrogen can cause an increase in water retention and weight gain.
Follicle stimulating hormone (FSH) increases, as the pituitary stimulates new follicles to mature. This increases oestrogen levels too. But high oestrogen also increases thecal cell proliferation, and so a vicious cycle starts.
Excessive LH, FSH, the androgens and oestrogens all suppress ovulation. Unless this occurs progesterone is not made. All this of course plays havoc with the ovaries, and emotions too.
Supplementing with progesterone suppresses the excess LH, FSH, oestrogen and testosterone, and helps regulate the cycle.
Contraceptives cause oxidative stress which leads to inflammation. Antioxidants are an essential part of establishing normal functioning ovaries.
As ovulation is suppressed, progesterone production stops, levels drop which can lead to depression. Often a diagnosis of depression is made, with no thought to the cause, so antidepressants are prescribed.
All contraceptives have the ability to cause insulin resistance, leading to tiredness, weight gain, a foggy brain and more.
The potential for blood clots increases, as oestrogen is known to cause platelets to aggregate.
"This study underscores the fact that prolonged and extensive use of these drugs in our daily life may be hazardous and also, that OC users should be aware of multifactorial risk factors (environmental, genetic and life style patterns) that may be responsible for additional DNA damage."
Progesterone can be used concurrently with contraceptives, and should be used during the progestin phase of the tablet pack. If a patch, implant or injection is used, progesterone can be used daily.
Progesterone
- prevents platelets aggregating and reduces thrombin by 10-15%, thereby preventing clots
- reduces atherosclerosis and plaque build up. It also prevents cholesterol from forming cholesteryl ester, a more potent form and increases biliary cholesterol output by the liver
- raises levels of serotonin and dopamine, thereby helping in contraceptive induced depression
- activates the GABA receptor sites. GABA is one of our most calming neurotransmitters, reversing anxiety and panic attacks
- activates the gene p53, often called the 'guardian of the genome', as it prevents cells multiplying and getting out of control as in cancer
- is a potent anti-inflammatory, raising levels of the anti-inflammatory Th2 cytokines
- is a vasodilator, relaxing blood vessels so reducing blood pressure
- is a bronchodilator, essential for normal lung function and preventing asthma
For more information on progesterone please see the web page on How to use progesterone.
Women should use between 100-200mg of progesterone daily.
Before using progesterone it's essential to first read the page on Oestrogen Dominance.
Please see here for more information on Nutrition and Diet.
For further reading see...
- Progesterone and Cancer
- Toxins in skin care
- Endocrine disruptors, Our Stolen Future
- Toxins in sunscreens
For more info on oestrogen or oestrogen/progestin combos, please see the HRT web page.
Websites on contraceptives...
Websites on HRT...
References
MedPage Today May 2012
Estrogen a Culprit in Inflammatory Bowel Disease
Medscape Jan 2012
US Group Seeks Re-Vote on Drospirenone Clot Risk
Gynecological Endocrinology, July 2006; 22(7): 355361
Medroxyprogesterone acetate exacerbates glutamate excitotoxicity
Carcinogenesis, Vol. 24, No. 5, 991-1005, May 2003
Predictors of the plasma ratio of 2-hydroxyestrone to 16-hydroxyestrone among pre-menopausal, nulliparous women from four ethnic group
The Lancet, Volume 346, Issue 8990, Pages 1593 - 1596, 16 December 1995
Enhancement by factor V Leiden mutation of risk of deep-vein thrombosis associated with oral contraceptives containing a third-generation progestagen
The Lancet, Volume 344, Issue 8935, Pages 1453 - 1457, 26 November 1994
Increased risk of venous thrombosis in oral-contraceptive users who are carriers of factor V Leiden mutation
Journal of Internal Medicine Volume 231, Issue 5, pages 561565, May 1992
Protracted cholestasis probably induced by oral contraceptive
Cochrane Fertility Regulation Group Issue 6, 2010
Copper containing intra-uterine devices versus depot progestogens for contraception
University of Missouri 2010
Breast Cancer Risk Varies Among Different Progestins Used in Hormone Replacement Therapy, MU Researchers Finds
Endocrine-Related Cancer 2009, 16 (1) 85-98
Regression of progestin-accelerated 7,12-dimethylbenz[a]anthracene-induced mammary tumors in Sprague-Dawley rats by p53 reactivation and induction of massive apoptosis: a pilot study
ScienceDaily (Mar. 11, 2008)
Certain Oral Contraceptives May Pose Health Risks, Study Suggests
The Global Library of Women's Medicine 2008
Pharmacology of Contraceptive Steroids
Medscape November 16, 2007
Oral Contraceptive Use Linked to Small Increase in Cervical Cancer Risk
Metabolism Volume 56, Issue 6, June 2007, Pages 830-837
Addition of medroxyprogesterone acetate to conjugated equine estrogens results in insulin resistance in adipose tissue
Diabetes Care 29:613-617, 2006
Long-Acting Injectable Progestin Contraception and Risk of Type 2 Diabetes in Latino Women With Prior Gestational Diabetes Mellitus
Maturitas Volume 49, Issue 4, 10 December 2004, Pages 315-320
Effects of progestins on estrogen-induced increase in C-reactive protein in postmenopausal women
International Journal of Obesity (2004) 28, 998-1003
Association between C-reactive protein, metabolic cardiovascular risk factors, obesity and oral contraceptive use in young adults
Journal of Thrombosis and Haemostasis Volume 2 Issue 9 Page 1594-1600, September 2004
Impact of progestagens on activated protein C (APC) resistance among users of oral contraceptives
Journal of Thrombosis and Haemostasis Volume 1, Issue 7, pages 1371&Mac226; 1380, July 2003
Estrogens, progestogens and thrombosis
Volume 46, Supplement 1, Pages 7-16 (10 December 2003)
Classification and pharmacology of progestins
Diabetes Care 26:216-225, 2003
Effects of Injectable or Implantable Progestin-Only Contraceptives on Insulin-Glucose Metabolism and Diabetes Risk
Best Practice & Research Clinical Obstetrics & Gynaecology Volume 17, Issue 3, June 2003, Pages 509-528
Thrombophilias and gynaecology
Mutat Res. 2002 Nov 26;521(1-2):113-9
Assessment of DNA damage in women using oral contraceptives
Thorax 2001;56:613-616
Exogenous female sex steroid hormones and risk of asthma and asthma-like symptoms: a cross sectional study of the general population
BMJ 1999;318:96-100 (9 January)
Mortality associated with oral contraceptive use: 25 year follow up of cohort of 46 000 women from Royal College of General Practitioners' oral contraception study
J Microbiol Immunol Infect. 1998 Sep;31(3):197-9
Premenstrual asthma: report of a case with hormonal studies
Human Reproduction, 1998, Vol 13, 3379-3383
The effect of a levonorgestrel-releasing intrauterine system on uterine artery blood flow, hormone concentrations and ovarian cyst formation in fertile women
Annals of Allergy, Asthma and Immunology, Volume 81, Number 3, September 1998 , pp. 243-246(4)
Exacerbation of Premenstrual Asthma Caused by an Oral Contraceptive
BJOG Volume 105 Issue 10 Page 1082 - October 1998
A double-blind randomised placebo controlled trial of postnatal norethisterone enanthate: the effect on postnatal depression and serum hormones
ScienceDaily (Apr. 16, 1997)
Pregnancy, Oral Contraceptives, Hormone Replacement Therapy As Risk Factors For Stroke
J Natl Cancer Inst (1995) 87 (11): 827-835
Oral Contraceptives and Breast Cancer Risk Among Younger Women
The American Journal of Medicine 1995, Volume 98, Issue 1, Supplement 1, Pages S104-S110
The androgenicity of progestins
The Lancet, Volume 344, Issue 8934, Pages 1390 - 1394, 19 November 1994
Oral contraceptive use and adenocarcinoma of cervix
Journal of Internal Medicine Volume 231, Issue 5, pages 561&Mac226; 565, May 1992
Protracted cholestasis probably induced by oral contraceptive
Journal of Steroid Biochemistry Volume 28, Issue 4, October 1987, Pages 379-384
Analysis of the androgenic activity of synthetic 'progestins' currently used for the treatment of prostate cancer
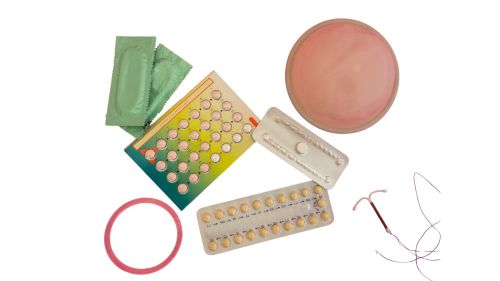 Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive…
Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive… We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c…
We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c… Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…
Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea… Endometriosis is a perplexing and often distressing condition affecting an estimated one in five women during their reproductive years. It occurs when tissue similar to the endometrium — the lining of…
Endometriosis is a perplexing and often distressing condition affecting an estimated one in five women during their reproductive years. It occurs when tissue similar to the endometrium — the lining of…