Cure for hot flashes
Before researching any potential cure for hot flashes, first lets define some terms... American English: Hot flashes (Dictionary definition: a thing that occurs suddenly and within a brief period of time). Standard English: Hot flushes (Dictionary definition: a reddening of the face or skin).
Normal flushing is the body responding to physical conditions such as exercise, hot temperatures, spicy food, alcohol, embarrassment or anger. It also occurs when the body over heats as in a fever, heat exhaustion, heat stroke, allergic reactions and inflammatory conditions.
Normal oral body temperature in adult men and women ranges between 33.2 - 38.2 C (92 - 101 F). Typical average temperatures are 37.0 C (98.6 F).
In women it varies between the follicular and the luteal phase. During the follicular phase, i.e. from the first day of menstruation to ovulation, it ranges from 36.45 to 36.7 C (97.6 to 98.1 F).
During the 12-14 day luteal phase, i.e. after ovulation to menstruation, temperature increases by 0.15 - 0.45 C (0.2 - 0.9 F) due to the increased metabolic rate caused by rapidly rising levels of progesterone. Temperature ranges between 36.7 - 37.3C (98.1 - 99.2F) during the luteal phase, but drops down to follicular levels within a few days of bleeding.
During a hot flush it is thought that a sudden stimulus to the temperature control centre within the hypothalamus causes it to go out of control, which gives a pointer to a possible cure for hot flashes. This stimulus also affects blood pressure (BP), sleep and anxiety too. Hot flushes and night sweats are associated with higher BP, disturbed sleep and anxiety.
The stimulus can be the result of...
- a sudden drop in hormones
- a rapid drop in the blood glucose level
- stress
- carcinoid syndrome
- chronic lymphocytic leukemia
- systemic mast cell disease
- tamoxifen
- pheochromocytoma
- medullary carcinoma of the thyroid
- pancreatic islet-cell tumours
- renal cell carcinoma
- hyperthyroidism
- neurological flushing
- somatostatinoma
The problem can be further aggravated by a hot drink, coffee or wine. Possibly because these disturb blood glucose.
The skin is the body's main defence against rising internal temperature, hence the flushing and/or sweating that occurs when it overheats.
But at present there is an incomplete understanding of the physiology of hot flushes which limits the search for a cure for hot flashes.
Although ascribed to an oestrogen deficiency in women, hot flushes do not occur in pre-pubertal girls, women with Turner's syndrome, unless taking oestrogen and older menopausal women. All who have little to no oestrogen.
Young women with ovarian dysgenesis, and therefore very low levels of oestrogen, never have hot flushes unless first given oestrogen.
The evidence suggests that the mechanism behind hot flushes is far more complicated than a decline in oestrogen, and that the neuroendocrine system is involved.
This includes corticotropin-releasing hormone (CRH), thyrotropin-releasing hormone (TRH), calcitonin gene-related peptide (CGRP), adrenaline (epeniphrine American), noradrenaline (norepeniphrine American), serotonin, endorphins, oestrogen, testosterone and progesterone, which all play a role.
Within the brain lies the hypothalamus. This controls blood pressure, body temperature, hunger, thirst, water balance, and is involved in sleep and emotional activity. It links the nervous system to the endocrine system by secreting neurotransmitters, neuromodulators and neurohormones.
One simple neurohormone is TRH. It's involved in the control of temperature, as it controls energy homeostasis. TRH causes wakefulness and loss of appetite. It's also found in pancreatic islets and the gastrointestinal tract, where it increases motility, notably in women with irritable bowel syndrome. It's released when stressed in an effort to keep the body in homeostasis.
TRH stimulates the pituitary to secrete prolactin. Excess levels of TRH inhibit dopamine, which also causes prolactin to increase. Excess oestrogen causes prolactin to rise too. Excess prolactin inhibits dopamine. Although prolactin is the hormone of lactogenesis, it's also an inflammatory hormone. A drop in dopamine can lead to anxiety and depression.
TRH also stimulates the release of noradrenaline from the frontal cortex, and the pituitary to release thyroid-stimulating hormone (TSH).
TSH stimulates the thyroid to secrete thyroxine and triiodothyronine which control the bodys metabolic rate, heat generation, neuromuscular function and heart rate.
But it appears that the production of nitric oxide (NO) may control the activity of the hypothalamus-pituitary-thyroid axis. NO is the intercellular signal that controls vascular tone (hence blood pressure), insulin secretion, airway tone, and peristalsis. Inhibition of NO decreases production of TSH, which reduces thyroxine and triiodothyronine and therefore the metabolic rate and temperature. The brain sensing this stimulates the secretion of TRH which would in turn increase metabolic rate and temperature. If this was too sudden, the body would overheat.
Noradrenaline is also associated with activation of the hypothalamic-pituitary-thyroid axis. It's also involved in the protein biosynthesis and secretion of TRH.
Progesterone stimulates the production of NO and suppresses noradrenaline. A drop in progesterone production would inhibit the release of NO and cause noradrenaline to rise.
Another neurohormone secreted by the hypothalamus is CRH. It's released in response to stress, whether physical or emotional, external or internal. CRH in turn stimulates the pituitary to release corticotropin, also called adrenocorticotropic hormone (ACTH). This in turn stimulates the adrenals to secrete cortisol, and together with the sympathetic nervous system and certain precursor chemicals, adrenaline and noradrenaline, the three stress hormones.
CRH also suppresses appetite, increases anxiety and improves memory and selective attention. It increases throughout pregnancy being produced by the foetus and placenta. It's thought that this increase ultimately starts labour. It's found in the gut, where it can initiate inflammation.
CRH is inhibited by progesterone, but excess CRH suppresses progesterone. An excess is also associated with depression, anxiety, sleep disturbances and anorexia. It can worsen, or possibly play a role in inflamed conditions such as arthritis, psoriasis, ulcerative colitis and Crohn's disease.
Progesterone levels rise sharply in pregnancy, suppressing CRH. But eventually the rising level of CRH from the foetus and placenta suppress progesterone, and labour starts.
Although hot flushes and night sweats are generally associated with Peri-menopause and the early years of Menopause, they can occur during puberty and while pregnant. They have been known to occur the few days before menstruation, which is when progesterone and oestrogen levels drop. It's only when the ratio of the two become skewed, i.e. excess oestrogen in ratio to progesterone that hot flushes would occur.
Hot flushes are generally worse towards the end of peri-menopause and in the early years of menopause. During the transition about 50% of women experience them, and can continue to do so for several years.
Severe symptoms can be experienced in women who have an early menopause, or who have had an oophorectomy, chemo or drug induced menopause.
Although menopause is associated with loss of ovarian oestrogen production, little cognisance is taken of the loss of progesterone in the preceding years. Or the loss associated with women who've had an oophorectomy, chemo or drug induced menopause.
Menopause is associated with a significant increase in the oestrogen related cancers, breast and endometrial. These tissues, together with adipose cells are important sites of postmenopausal oestrogen production.
The capacity of adipose cells to produce oestrogen increases significantly with age. But there is no corresponding increase in progesterone production. Surely the rationale behind hot flushes, breast and endometrial cancer too, would be the drop in progesterone, and not oestrogen. Particularly when one takes into account hot flushes begin in peri-menopause when oestrogen levels are still high. Herein lies a pointer to a cure for hot flashes.
CGRP is a vasoactive, pro-inflammatory neuropeptide implicated in the pathogenesis of cardiovascular disease. Elevated levels increase the risk of hyperinsulinemia and cardiovascular disease in postmenopausal women. It causes an increase in blood pressure, a rise in noradenaline and a lowering of gastric secretions. It decreases motility and contraction of the gut.
It's implicated in migraine and cluster headaches and causes neurogenic inflammation. CGRP degranulates mast cells which release various chemicals triggering inflammation. Progesterone inhibits mast cell secretions.
Increased levels of CGRP are found in postmenopausal women compared with premenopausal women. Adipose cells are important for the production of CGRP, with increased levels seen in the abdominal subcutaneous fat in postmenopausal women. Adipose cells are also the main site of oestrogen production in these women. Oestrogen stimulates adipose cells to divide and multiply, so a vicious cycle starts.
Elevated CGRP levels are found particularly during hot flushes. They can be found in pregnancy too, which suggests that oestrogen and progesterone may influence their secretion.
Men also experience hot flushes. These can be caused by low testosterone, particularly in older men going through andropause. But it's more likely to occur in those on anti-androgen therapy for prostate or testicular cancer, or after removal of the testes.
A few studies have found CGRP is involved in hot flushes in men who had castration or androgen deprivation therapy due to prostate cancer. One study found ovarian hormones and testosterone inhibited CGRP.
Flushes can last from 0.5 to 60 minutes, but generally 3 to 6 minutes, with the average being 3.3 minutes.
If some substance causes adrenaline and noradrenaline to rise, it provokes a hot flush. The converse is true, if a substance causes a reduction, it ameliorates a hot flush.
The major triggers of adrenaline and noradrenaline release are physical threat, excitement, noise, bright lights, a drop in blood glucose and high ambient temperature.
Adrenaline and noradrenaline are part of the fight-flight response. As such they increase vascular tone, ie constricts blood vessels, cause the heart to beat faster, trigger the release of glucose from glycogen (stored glucose), and increase oxygen to the brain. This has the effect of increasing heat within the body.
Serotonin levels in post menopausal women can drop by 50%. There are 13 sub-types of serotonin receptors, but for the purposes of this page, only 5-HT 1A and 5-HT 2A will be mentioned.
5-HT 2A causes neuronal excitation and is implicated in hot flushes. It also causes behavioural effects, platelet aggregation and anxiety. If 5-HT 2A receptors increase, it's thought to cause a change in body temperature. This causes the autonomic system to switch on to try to cool the body down.
It does this via 5-HT 1A which dilates blood vessels in the skin. This increases heat dissipation from the body out into the environment, causing sweating and a decrease in body temperature. It also causes a decrease in blood pressure, heart rate and anxiety.
Interestingly, progesterone is a potent vasodilator, it's also thermogenic, which would increase skin temperature, particularly if a transdermal application was used. It's also an anxiolytic, thereby reducing anxiety.
The current thinking is that reduced oestrogen levels cause 5-HT 2A to increase. But it's not listed amongst the antagonists which decrease 5-HT 2A.
Antagonists of 5-HT 2A, such as some SSRI antidepressants, reduce hot flushes. Whereas activation by an agnonist upsets the thermoregluatory system and causes a hot flush. The psychedelic drugs like LSD, psilocin and mescaline, act as agonists on the receptor.
The prevalence of nighttime hot flushes could be due to the drop in serotonin due to it's conversion to melatonin. There is a slight improvement with the use of SSRI's, but the side effects are in some cases, the same symptoms that are experienced with hot flushes.
5-HTP reduced hot flushes non-significantly in one study, but generally tryptophan is more effective than 5-HTP. Another small study found tryptophan depletion did not increase hot flushes. Depleting tryptophan defeats the purpose, increasing it would be more effective.
Sumatriptan, a 5-HT1 receptor agonist, is structurally similar to serotonin, and is used to treat increased CGRP levels in migraine by inhibiting it's release. An interesting concept would be to study whether serotonin or it's precursor tryptophan, would inhibit CGRP and provide a possible cure for hot flashes.
The nucleoside adenosine is a natural inhibitor of noradrenaline. Dopamine and serotonin also inhibit it. Progesterone is a mono amine oxidase inhibitor, thus preventing the breakdown of serotonin and dopamine. It also increases the release of adenosine.
Allopregnanolone, a metabolite of progesterone, is a potent anxiolytic and anti-inflammatory, which also increases dopamine levels.
Adrenaline and angiostensin stimulate noradrenaline release. Vitamin D inhibits angiotensin, progesterone inhibits adrenaline and noradrenaline.
So to recap...
- Hot flushes increase in severity and frequency during the last year or so of Peri-menopause. Progesterone is dropping precipitously during this period, as anovulatory cycles occur with greater frequency. But ovarian oestrogen does not drop until the last viable egg has completed it's growth. Furthermore, oestrogen in the form of oestrone, is still produced by adipose cells, these do not secrete progesterone to counter the oestrogen.
- An interesting point, but women with Turner's syndrome, or young women with ovarian dysgenesis, having very low levels of oestrogen, or none at all, never have hot flushes unless first given oestrogen. This makes one wonder if the reason is nothing more than excess oestrogen causing hot flushes, and not a drop in oestrogen as women are lead to believe. This is certainly supported by the fact that progesterone is dropping sharply during the last year or two of peri-menopause, but oestrogen is not.
- A sudden surge in adrenaline and noradrenaline can cause a hot flush. This surge can be provoked by blood glucose dropping too suddenly. This itself is often caused by eating or drinking something sweet.
- Stress, particularly sudden, causes a surge in the two hormones, see Anxiety.
- A drop in serotonin can cause a hot flush. This drop can occur because of stress, lack of the precursor amino acid tryptophan in the diet, or a reduced ability to convert tryptophan into serotonin. This last could be due to a lack of the necessary co-factors vitamin B6 and folic acid which drop when stressed, as do all the B vitamins.
- Excess CRH and TRH could possibly be implicated, released in response to stress.
- A high level of CGRP is found in menopausal women. An elevated level of CGRP is implicated in hot flushes, particularly during a hot flush. Men who've been castrated or are on anti-androgen therapy can have an increase in CGRP during a hot flush.
- Although high levels of CGRP have been found in pregnancy too, it seems likely the increase is due to excess oestrogen and not progesterone. This is certainly the case in peri-menopause with dropping progesterone levels. Oestrogen is an excitatory hormone, whereas progesterone is calming.
- Progesterone is a potent anxiolytic, in part due to it's action on the GABA receptor sites. GABA is a calming neurotransmitter. And in part because it inhibits the release of adrenaline and noradrenaline from the adrenals. It's also a monoamine oxidase inhibitor, so increasing serotonin and dopamine levels slightly. Plus it inhibits the release of CRH. All of which points to progesterone being a potential cure for hot flashes.
It seems highly likely that the disturbed ratio of progesterone to oestrogen is behind hot flushes in women. Possibly in men too who've been castrated or are on anti-androgen therapy, as the testes are a source of progesterone and testosterone.
As stated earlier, surely the rationale for hot flushes is dropping progesterone levels, and normal oestrogen levels. Supplemental progesterone is an effective cure for hot flashes, or reduces them considerably.
Hot flushes and night sweats are associated with higher blood pressure, cardiovascular risk, higher factor Vllc (a clotting factor), higher inflammatory markers, and are a marker for risk of adverse bone health. CGRP, CRF, prolactin and oestrogen are inflammatory hormones, often found in excess in peri-menopause and menopause.
Progesterone is an anti-inflammatory hormone, mainly due to it's metabolite allopregnanolone. It inhibits mast cell secretions, CGRP, CRF, prolactin and oestrogen, all inflammatory. It also inhibits platelet aggregation, which leads to increased clotting, and stimulates osteoclasts involved in bone formation. Being a potent vasodilator, it can reduce blood pressure, plus it increases the production of NO, itself a potent vasodilator.
Menopause is associated with an increased prevalence of Insulin Resistance and metabolic syndrome (MetS), which are risk factors for cardiovascular disease. There is a higher frequency of symptoms such as hot flashes and sweating in women with MetS.
Excess oestrogen is one of the causes IR. So is a lack of vitamin D.
In seeking a cure for hot flashes it's essential to reduce stress. And to keep blood glucose stable by avoiding all sugars, any food or drink containing sugar, and sweet, starchy foods which convert to sugar, ie grains, legumes or sweet fruits and vegetables that fall into this category.
Essential too to keep the ratio of progesterone to oestrogen high.
By reducing the stress response, which increases anxiety and inflammation, progesterone assists in regaining homeostasis.
One final note...
It seems all the more likely that high levels of oestrogen are responsible for hot flushes. As mentioned earlier, oestrogen causes the temperature to drop, and it will stay down if excess oestrogen is present.
The body sensing this sends out emergency messages to bring it up again, also noted above. It does this too effectively, the end result being a hot flush.
Much the same overreaction occurs if blood glucose drops too sharply. The brain sends an emergency message to the adrenals to make adrenaline to bring it up again. But the end result is a pounding heart and possible panic attacks.
Hot flushes and night sweats are associated with higher blood pressure, cardiovascular risk, higher factor Vllc (a clotting factor), higher inflammatory markers, and are a marker for risk of adverse bone health. Excess oestrogen is associated with all these.
Natural treatment/ Cure for hot flashes
- progesterone
- tryptophan/5-HTP
- deep breathing
- acupuncture
- yoga
- hypnosis
- salvia officinalis
Under normal circumstances, women require 100-200mg/day progesterone, unless symptoms are severe. Hot flushes, once started, only respond to levels of 400mg/day and over.
Men generally need 10-100mg/day progesterone, but 100mg/day and over will be needed to stop hot flushes.
Consider taking tryptophan, the precursor amino acid to serotonin, and tyrosine, the precursor amino acid to dopamine. This will raise dopamine levels which will inhibit prolactin production. See Anxiety.
Vitamin D is essential for the normal functioning of all cells. It's also a potent anti-inflammatory and antioxidant, consider having a test done.
For more information see these websites
Medical treatment
SSRI antidepressants
Clonidine an anti-hypertensive
Gabapentin an anticonvulsant
Alternative treatments to HRT include the following, all have non-significant effects...
Phyto-oestrogens in particular the isoflavones from soy, which have an oestrogenic effect.
Herbs such as dong quai, agnus castus, red clover, black cohosh, all oestrogenic.
Vitamin E
Reference websites...
Thyrotropin-releasing hormone (TRH)
Corticotropin-releasing hormone (CRH)
Adrenocorticotropic hormone (ACTH)
References for cure for hot flashes
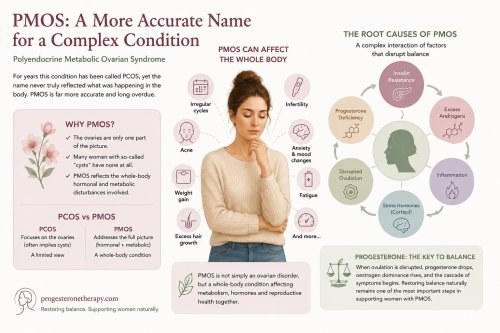 For years this condition has been called PCOS, yet the name never truly reflected what was happening in the body. The ovaries are only one part of the picture. Many women with so-called “cysts” have n…
For years this condition has been called PCOS, yet the name never truly reflected what was happening in the body. The ovaries are only one part of the picture. Many women with so-called “cysts” have n… Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive…
Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive… We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c…
We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c… Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…
Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…