Progesterone and Conception,
Pregnancy and Contraception
Extract taken from Dr Katherina Dalton's book 'PMS The Essential Guide to Treatment Options'
Chapter 13
It is a well-recognized fact about PMS that most sufferers are free of their monthly problems when pregnant, or at least during the second half of pregnancy. This is because the placenta produces huge amounts of progesterone to keep the pregnancy going - it may raise the level of progesterone in the blood to 40 or even 50 times the greatest amount found in non-pregnant women. However, there are a few women who continue to experience their PMS symptoms daily during later pregnancy, and these women are the ones who are most at risk of developing pre-eclampsia (page 150).
CONCEPTION
Women who suffer from PMS usually have no difficulty in conceiving. When patients who are receiving progesterone therapy are ready to become pregnant, they are advised to start their usual course of progesterone two to four days later and continue until the pregnancy is confirmed. Then they should phone for further advice. They will be asked if they have any of the usual pregnancy problems - nausea, vomiting, headaches, excessive tiredness or depression. These are common symptoms in early pregnancy and can be relieved by increasing their current dose of progesterone.
If a woman is not experiencing any of these pregnancy symptoms, she can reduce her usual dose of progesterone slowly, week by week, on the other hand if these pregnancy symptoms are present, the patient should increase her dose of progesterone every few days until she feels really well. She will usually be asked to report her progress on the phone, week by week until the symptoms are stabilized. Often progesterone may be needed until the placenta is fully functioning and producing large amounts, which is generally about the fourth month. (See Figure 40 on page 154, which indicates the beneficial effects of progesterone on the children of mothers given progesterone in early pregnancy.) Recent advances in the use of ultrasound pelvic scans have revealed just how often conception occurs only to be followed by failure of the fertilized ovum to embed itself into the lining of the womb, even in perfectly normal, fertile women. This results in an early miscarriage even before the woman has considered the possibility of a pregnancy, or it may even happen as early as the time of the next expected period. The only telltale sign may be unexpectedly heavy menstrual bleeding and/or more pain than usual.
Defective Luteal Phase
Progesterone is the pregnancy hormone. If there is too short an interval between ovulation and menstruation, this is known as a defective luteal phase. The short interval, of less than 12 days, means that there has not been a high enough progesterone level and this may result in an early miscarriage, due to failure of the fertilized egg to embed itself in the lining of the womb. This hazard can be overcome by ensuring there is sufficient progesterone after ovulation and until the placenta has started producing enough on its own. It means continuing progesterone therapy until about the fourth month of pregnancy.
In Vitro Fertilization
Those unfortunate women who, for one reason or another, have difficulty in conceiving naturally and need in vitro fertilization (IVF) will also require progesterone from the time of implantation until the placenta is producing enough progesterone to keep the embryo going. There are several different types of IVF treatment, but they will all need plenty of progesterone in the first few weeks.
PREGNANCY
Morning Sickness
Morning sickness in early pregnancy is another hazard for PMS sufferers. In fact, many will tell you that the name is wrong -they are sick all day, not just in the morning. When this problem is severe it is called hyperemesis (from the Greek words hyper, meaning 'excessive' and emesis, meaning 'vomiting'). This seems to mean that in former times doctors (who were always male, of course) considered mild vomiting in early pregnancy to be quite natural, something to be expected and which the women should learn to accept. It's a pity they never had to go through it. In fact it is caused by a hormonal imbalance before the placenta is fully formed, and usually improves by about the 16th week of pregnancy. Using progesterone will help this problem, too.
Habitual Miscarriages
When a woman has had several miscarriages, she is naturally anxious that everything medically possible is done to ensure that she has a normal full-term pregnancy - and, not surprisingly, she will often be given progesterone therapy to ensure this. There are many causes of miscarriages, including chromosomal defects, about which little can be done at present, but they may be due to anatomical abnormalities such as a lax cervix (opening to the womb), which can be stitched up until labour starts. There are also women who suffer from excessive vomiting and pregnancy symptoms immediately they become pregnant, and these are the ones most likely to benefit from progesterone given in a dose high enough to remove their symptoms. Among many patients thus treated over the years, the author has treated two women who had both had nine previous miscarriages and who were both given progesterone therapy; both were later delivered successfully of healthy babies at the City of London Maternity Hospital.
Threatened Miscarriages
Bleeding in early pregnancy is always a worry; the patient is naturally wondering whether it is the end of the pregnancy or not. if the bleeding is scanty and does not contain clots or fetal tissue, then with rest there is a chance that all will be well and that a normal pregnancy will continue. This applies particularly if the bleeding comes at the expected time of the first missed period. If it is accompanied by excessive vomiting and early pregnancy symptoms, then again the patient will benefit from progesterone therapy in a dose sufficient to ease the symptoms. However, after the delivery the doctor is left wondering if the pregnancy would have continued even if progesterone had not been given.
Pre-eclampsia
Pre-eclampsia was previously known as 'toxaemia of pregnancy' and is often referred to as PET, or pre-eclamptic toxaemia. The word toxaemia means 'blood-poisoning'; pre means 'before', and the eclampsia refers to the convulsions which can sometimes occur in severe cases of PET, often resulting in the death of the mother or the baby. It is still one of the commonest causes of both infant and maternal deaths in Britain and throughout the world.
We still don't know exactly what causes PET, although all over the world scientists are searching for a better understanding of the disease process. It is known that harmful changes occur in the endothelial cells (the cells lining the inside of blood vessels) of the womb and placenta, where plaques begin to form between the 16th and 20th week of pregnancy, but the disease does not show until late pregnancy when there is a rise in blood pressure, excessive weight gain, swelling of the ankles and protein in the urine.
In the first-ever description of 'Premenstrual Syndrome', in the British Medical Journal in 1953 by Dr Raymond Greene and this author, it was noted that twice as many PMS sufferers had been hospitalized because of pre-eclampsia in a previous pregnancy compared with the normal number of cases of pre-eclampsia in the general population. This led to a survey of 825 women, published in the British Medicaliournal in 1955, which confirmed that the 192 women who had previously suffered from pre-eclampsia had a 86 per cent incidence of PMS compared with 27 per cent among those whose pregnancy had been normal (Figure 39). This suggested a link between pre-eclampsia and PMS.
The women in the survey were interviewed personally by the author, who noted that the symptoms experienced by those who had pre-eclampsia during middle and late pregnancy were the same as those which they subsequently experienced during their PMS. For instance, the biggest problem for some women was headaches throughout pregnancy, and these women were later troubled by premenstrual headaches; others were worried by depression or backache, in each case it was these same symptoms which later caused problems before their periods.
In the 1950s, a few women with severe PMS including premenstrual epilepsy, asthma and migraine, were tested daily for weight, blood pressure and protein in their urine, the same tests as are done during antenatal examinations in order to spot PET. These examinations showed that women with severe PMS also had an increase in weight, blood pressure and developed protein in their urine before menstruation, but these measurements were normal after menstruation. These patients were then treated with daily progesterone injections and the daily examinations continued, but with progesterone there was no weight gain, no rise in blood pressure and no protein in the urine. They were free from symptoms.
In another survey by this author, published in the Lancet in 1960, 640 women attending the antenatal clinic of University College Hospital, London, were asked between the 16th and 28th weeks of their pregnancy whether they felt as well as they did before they became pregnant. Their names and hospital number were then entered either into a book marked 'YES' or one marked 'NO'. The patients' records were later studied and it was found that among those women who felt ill during the middle months of pregnancy, 25 per cent developed pre-eclampsia compared with only 10 per cent among those who felt well. The complaints of the women who were not feeling well in the middle months of pregnancy, and who later developed pre-eclampsia, are shown here:
Symptoms in the middle months of pregnancy in those who later developed pre-eclampsia...
- Lethargy 88 per cent
- Backache 44 per cent
- Headache 35 per cent
- Nausea and vomiting 65 per cent
- Vertigo 26 per cent
- Depression 52 per cent
- Fainting 12 per cent
These facts all suggested that there was a marked similarity between pre-eclampsia and PMS - in fact, in the days when pre-eclampsia was called 'toxaemia of pregnancy', it was suggested that PMS should be called 'toxaemia of menstruation'. Both have an early first stage of symptoms, followed in severe cases by the second stage of weight gain, rise in blood pressure and protein in the urine, and if the disease progresses even further there is a third stage of fits, either eclamptic convulsions or epileptic fits.
Similarity of PMS and pre-eclampsia...
- First stage
- Nausea and vomiting
- Irritability
- Lethargy
- Backache
- Depression
- Fainting
- Headache
- Second Stage
- Weight gain
- Rise of blood pressure
- Swelling of ankles and fingers
- Protein in the urine
- Third Stage
- Epileptic fits, preceded by severe headache
- Eclamptic convulsions, preceded by severe headache
Because progesterone is successful in PMS if used early, it was decided to use progesterone in controlled trials for pre-eclampsia, first by injection (1962) and later by suppository (1972).
Volunteers attending the antenatal clinic of Chase Farm Hospital, Enfield, who were in the middle months of pregnancy and complaining of pregnancy symptoms, were allocated randomly to receive either progesterone or treatment which would relieve their symptoms until they were well again or until their baby was born. It proved easy enough to relieve symptoms in both groups of 296 pregnant women, but in the group of those receiving progesterone only 3 per cent developed pre-eclampsia, compared with the symptomatic treatment groups in which 11 per cent developed pre-eclampsia.
Progesterone treatment for pre-eclampsia has proved effective in Egypt and Japan, but in Britain doctors have feared that progesterone in pregnancy would have the same harmful effects on the fetus as the artificial man-made progestogens. Also, in Britain consultant obstetricians do not usually see antenatal patients until the late stage of pregnancy, when they would much prefer to have proof of tests showing abnormal blood pressure and protein in the urine, rather than rely on a woman's account of how she feels.
Antenatal Progesterone and the Foetus
In the late 1950s pregnant women suffering from morning sickness were successfully treated with progesterone injections. Several of these children were in the author's general practice. One morning a patient asked me if I had attended the local school's prize-giving the previous day. When I asked 'Why?' I was told that I had delivered many of the prize winners. This roused my curiosity, and at coffee break the files of the named prize winners were fetched out and looked at. I noticed with surprise that the prize winners' mothers had received progesterone for morning sickness during their pregnancies.
The local Director of Education was most interested and asked for a list of 40 local children, including the six prize winners and others who had received progesterone in the womb. He checked with the headmasters if the other 'progesterone children' were also bright. Indeed, a lot of the children who received progesterone in the womb appeared to be brighter than average.
There then followed a full-scale survey of the children of all mothers who had received progesterone at the City of London Maternity Hospital between 1959 and 1961. The children were then 9-10 years old and scattered around London and various parts of Britain, and they were each matched with a 'control' -the next baby in the labour ward register. The babies' progress could then be compared with these controls. The school heads were asked to grade each child as average, below average or above average in English, arithmetic, verbal reasoning, craftwork and physical education (Figure 40).
Further results confirmed that among the 'progesterone children', the best results were among those who received high doses compared with low doses, long courses compared with short courses and before the 16th week of pregnancy compared with later in pregnancy. This was true in all the academic subjects: English, arithmetic and verbal reasoning but not in physical education or craftwork. In medical terms, the results showed that the effect of progesterone on intelligence was 'dose related' - the more the better.
The children were followed up until the age of 20 years, when they showed better exam (0 and A level) results than did the controls. Finally, 32 per cent of the 'progesterone children' went on to university, compared with only 6 per cent of the controls, and 6 per cent is also the average number for the borough of Haringey and the Inner London Education Authority who entered university during those years (Figure 41). Although the survey has now finished I can record anecdotally that the 'progesterone children' have married and have had no problems with fertility.
In 1960 the first reports appeared of abnormalities to a fetus exposed to progestogens - it was found that they caused masculinization of female babies. At that time. the differences between progestogens and progesterone were not well understood, so progesterone was no longer used for the relief of morning sickness in pregnancy. In retrospect, it is not surprising that these abnormalities occurred, as the progestogens then used were all related to the male hormone testosterone. However, with the arrival of in vitro fertilization ('test-tube babies') it has been recognized that progesterone is an essential hormone of pregnancy, and it has been given to women when the fertilized egg is planted in the womb and until the placenta is producing adequate progesterone. So, in the future we can hope to see more of these intelligent 'progesterone children'.
Postnatal Depression
Postnatal depression (PND) is really the wrong name for an illness which affects 10 per cent of new mothers after their baby's birth, because depression is rarely the first symptom to appear and in many cases there is never any depression at all. Women who have suffered from PND can give much better descriptions of how they felt at the beginning of their illness, describing the sleeplessness and feeling 'not with it' - 'distant' - 'shattered' 'confused' - 'losing touch' - 'muddled' - 'out of control' - 'high, gloriously high' - 'mind going round' - 'couldn't talk/wouldn't go out/kept the curtains drawn each day' - 'spent money like there was no tomorrow'- 'angry' and 'panicky'.
It can be a horrifying experience for a partner to come face-to-face with the changed personality of the new mother who was previously calm and is now so anxious, previously alert and active but now dull and speechless, previously a successful career woman and now frightened to be left alone, previously carefree and now obsessional. As mentioned previously, postnatal depression, and its more severe cousin puerperal psychosis, are hormonal diseases which have a lot in common with PMS and frequently turn into PMS as time passes. As a PND sufferer gradually improves, she will find that her symptoms get better after menstruation, only to get worse again before the next menstruation, and with further progress she gradually reaches the stage when there is absence of symptoms after menstruation but many of the symptoms premenstrually. At this point the illness has changed to PMS.
Postnatal depression tends to occur in women who have suffered from severe PMS and in those who have already suffered from postnatal depression or puerperal psychosis after a previous pregnancy, and it may come unexpectedly after a perfectly normal pregnancy and delivery. It can be successfully avoided if arrangements are made during the pregnancy with the general practitioner, obstetrician and midwife. After the baby has been safely delivered, the mother should be given the first of seven daily progesterone injections: of 100 mg followed by 400 mg progesterone suppositories twice daily for the next two months or until normal menstruation returns.
Menstruation is not likely to return until after breastfeeding has finished, so if the mother is feeling well and plans to continue breastfeeding for many months, the progesterone can be stopped after two months - but, if the symptoms come back, the progesterone should be restarted. When progesterone was first isolated in 1934, researchers thought that its job in the body was to prepare the breasts for breastfeeding. Progesterone helps breastfeeding and mothers need not worry that it will upset their babies.
Progesterone for Postnatal Depression
Immediately after delivery, progesterone injections 100 mg daily for seven days, followed by progesterone suppositories 400 mg twice daily until the return of menstruation or for two months.
Good News...
When PMS sufferers have had adequate progesterone during pregnancy so that there have been no symptoms of pregnancy, no hyperemesis or rise of blood pressure, and if progesterone has been given after the delivery to prevent any postnatal depression, then there is about a 50:50 chance that the PMS will not return.
CONTRACEPTION
Contraception is often a problem for women with PMS. All contraceptive pills contain progestogens, and as has already been explained in Chapter 5, the artificial man-made progestogens lower the blood progesterone level and so increase the severity of PMS. This means that the Pill should be avoided. Again, it is known that PMS increases in severity after sterilization (see Chapter 1), so this rules out another popular method of contraception. The intra-uterine device, or IUD, is best not used by any woman who has had problems with pelvic infections or by young girls who have not been pregnant. Withdrawal as a method of contraception is very unreliable (and bad for the nerves!). So, apart from progesterone contraception, this leaves condoms - male or female - the diaphragm (or 'Dutch Cap') and vasectomy.
Nowadays a doctor would advise any woman with a new partner to use a condom for the first six months, until any risk of HIV or AIDS has passed.
Progesterone Contraception
Progesterone is as safe a contraceptive as the intra-uterine device or the progestogen-only pill, if used as follows...
Start on Day 8 of the cycle with a low dose of progesterone, and keep it up until menstruation or - for PMS sufferers - the day when you start on the bigger, anti-PMS dose. A daily dose of 100 mg (half a 200 mg suppository) or a 400 mg suppository are equally effective. (Many women who will use 400 mg of progesterone two to six times daily from ovulation onwards prefer to take one 400 mg suppository in the follicular phase rather than having to get 200 mg suppositories as well.)
Progesterone contraception for PMS...
- A low dose (100-200 mg) of progesterone from Day 8 of the cycle
- Increase to optimum progesterone dosage at ovulation
- Continue progesterone until menstruation
A study of progesterone contraception in women with severe PMS showed 15 failures in 253 women who had used progesterone contraception for an average of 5.82 years. This means a failure rate of 2.66 per 100 women/years (women/years is a ratio that encompasses 100 women using a method of contraception for one year, 50 women using it for two, etc.), which compares favourably with the recognized failure rate of the condom of 14, diaphragm of 12, rhythm method 24, and intra-uterine device of 2.5 per 100 women/years.
However, some women find that by starting progesterone early they start bleeding at, or shortly after, ovulation. They should be advised to lower the dose of daily progesterone from Day 8 to 100 mg daily and start their usual higher dose of progesterone about two days after ovulation. If extra bleeding still occurs, then it is best to use a condom or diaphragm until the normal time of starting their course of progesterone. Should attacks of diarrhoea occur when using progesterone, then contraception cannot be guaranteed and alternative methods are advised.
Here is a list of Dr Dalton's books with links to Amazon...
Depression after Childbirth: How to Recognise, Treat, and Prevent Postnatal Depression
Premenstrual Syndrome and Progesterone Therapy
Another book well worth reading was written by one of her patients. Nicola Owen, who's problems all started when she was fourteen and going through puberty, ended up in Holloway Prison for Women in the UK. Dr Dalton prescribed progesterone which corrected the psychosis, thereby helping her recover and obtain her release. It's now out of print, but Amazon do have second hand copies.
Nicola
by Nicola (with Sydney Higgins) Owen (Author)
To find out more on the subject of progesterone and conception, please click here.
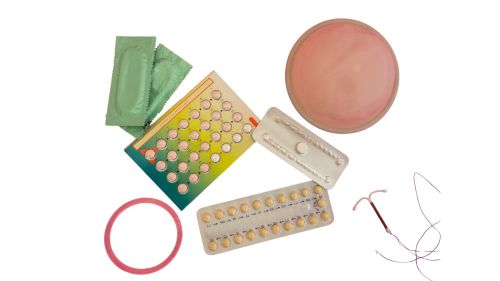 Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive…
Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive… We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c…
We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c… Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…
Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…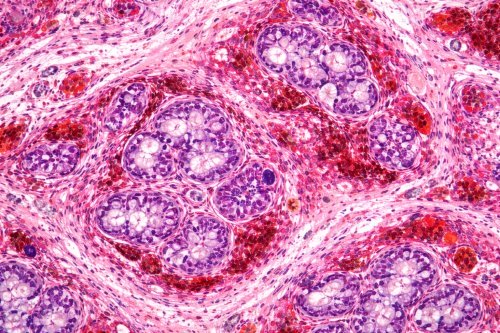 Endometriosis is a perplexing and often distressing condition affecting an estimated one in five women during their reproductive years. It occurs when tissue similar to the endometrium — the lining of…
Endometriosis is a perplexing and often distressing condition affecting an estimated one in five women during their reproductive years. It occurs when tissue similar to the endometrium — the lining of…