Seasonal affective disorder treatment
Normal seasonal affective disorder treatment is to make the sufferer extend the daylight hours with artificial lighting. This condition, also known as SAD, is caused by the long nights experienced in higher latitudes. The depression associated with late autumn and winter is thought to be caused by a lack of light.
Some of the symptoms of SAD are...
- depression
- weight gain
- cravings
- panic attacks
- lack of energy
- low libido
All of which are of particular interest as progesterone is involved in stabilising blood glucose, in calming, in increasing metabolism, in reversing depression and in increasing libido and energy. Excess oestrogen would exacerbate the situation.
Progesterone levels drop during dull or cloudy days which indicates it could be a useful seasonal affective disorder treatment. This is particularly noticeable in higher latitudes during the winter months.
Low levels of vitamin D affect the benefits of progesterone too, which explains why dark, cloudy days and winter affect progesterone levels, as they also drop vitamin D levels.
Interestingly more women are affected by SAD than men. This is not surprising as women suffer many more problems than men. Inflammatory and autoimmune diseases are far more prevalent in women.
Very little cognisance is given to the higher oestrogen levels in women compared to men as a possible reason. The incidence for these disorders is higher during the Peri-menopause years with dropping progesterone levels.
SAD only occurs in the winter months and is normally treated with light therapy. Although this can be affective, many hours are needed in front of a bright light for a reversal of symptoms.
Of far more importance would be increasing vitamin D levels, by either using a sun bed (which also gives light of course) or taking vitamin D supplements.
Supplemental progesterone is called for too. A 2009 study found a lack of vitamin D reduces the benefits of progesterone.
Brain-derived neurotrophic factor (BDNF) is low in depressed and suicidal people. BDNF is a neurotrophin which plays an important role in the regulation and growth of neurons, with important implications in neuronal survival and axonal regeneration. Progesterone and vitamin D increase levels of BDNF.
Many diseases and disorders vary between summer and winter. All pointing to low vitamin D levels in winter.
The weight gain can be ascribed to higher adipose tissue lipoprotein lipase (ATLPL), which stores free fatty acids in adipose cells. ATLPL rises in winter. Total cholesterol is higher in the winter than in the summer too.
There is a definite variation of CVD between summer and winter, with a higher incidence in winter. This is particularly noticeable in the higher latitudes.
Cerebrovascular disease increases in winter, as do ischaemic heart disease, hypertensive disease, pneumonia and bronchitis. Mortality from these diseases is higher in winter and spring and low in late summer.
There is a common belief in the northern hemisphere that the increase is due to the holiday season, rather than to climatic factors, as cardiac and noncardiac mortality peaks around Christmas and New Year. There is a significant increase for individuals who are dead on arrival at a hospital, die in the emergency department, or die as outpatients over the Christmas/New Year's holidays.
A similar study conducted in Australia found the same incidence in coronary artery deaths. But occurring from June to August, peaking in July. This is winter in the southern hemisphere. Mortality rates did not increase during the Christmas and New Year holidays which is high summer in the southern hemisphere.
They speculate this could be due to respiratory infections which increase in winter, or a direct effect of cold, plus seasonal changes in lipid concentration. This last is true of course, as ATLPL and cholesterol rise in winter. But no thought was given to low vitamin D levels
A further northern hemisphere study found an increase in hip fractures for both sexes during winter, with a peak occurring during November to February. They ascribe the difference to temperature, with little thought about the sun and vitamin D production.
Many studies have found a correlation between depression, respiratory infections, heart disease, increased weight gain and more, with low vitamin D levels.
Progesterone is also protective against the symptoms of SAD, heart disease, respiratory disorders and more. Combined with vitamin D the effect is amplified.
Both progesterone and vitamin D regulate gene expression, have a positive fundamental effect on cell differentiation and growth, with anti-oxidative and autoimmune anti-inflammatory mechanisms. Both positively effect the nervous system by stimulating neurotrophic factors, quenching oxidative hyperactivity and regulating autoimmune responses.
See Progesterone and Vitamin D.
Natural seasonal affective disorder treatment
The amount of progesterone will be dependant on the individual and the severity of the problem. Women should use between 100-200mg of progesterone daily, men should use between 10-100mg/day. In severe cases more might be needed, vary the amount used following symptoms as a guide.
For more information see... How to use progesterone cream.
Before using progesterone it's essential to read the page on Oestrogen dominance first.
A vitamin D test is essential. A lack of vitamin D reduces the benefits of progesterone. Blood levels should be 70-100ng/ml or 175-250nmol/L and not the 30ng/ml or 75nmol/L most labs and doctors regard as adequate. The minimum daily dose should be 5000iu's per day, although the latest research indicates it should be 10,000iu's per day, see here.
For more info on vitamin D levels, test kits etc see...
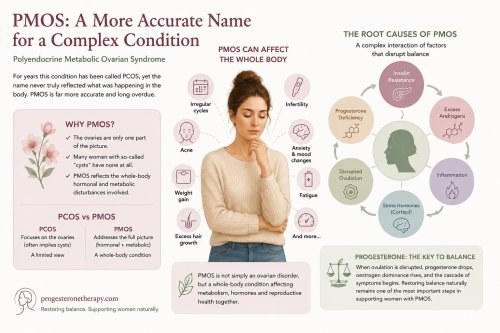 For years this condition has been called PCOS, yet the name never truly reflected what was happening in the body. The ovaries are only one part of the picture. Many women with so-called “cysts” have n…
For years this condition has been called PCOS, yet the name never truly reflected what was happening in the body. The ovaries are only one part of the picture. Many women with so-called “cysts” have n…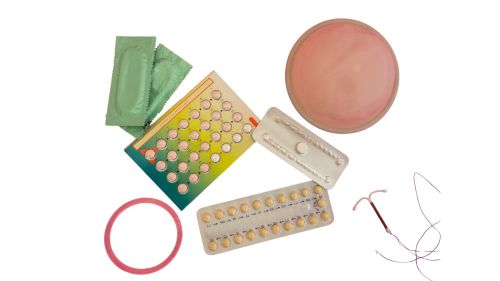 Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive…
Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive… We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c…
We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c… Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…
Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…