Contraceptives research papers
Estrogens, progestogens and thrombosis
Departments of *Clinical Epidemiology, †Haematology, ‡Gynaecology and Reproductive Medicine, Leiden University Medical Center, the Netherlands
Contraceptives May Pose Health Risks, Study Suggests
ScienceDaily (Mar. 11, 2008) - The widely used synthetic progestin medroxyprogesterone acetate (MPA) decreased endothelial function in premenopausal women in a study done at the University of Oregon. The finding, researchers said, raises concerns about long-term effects of MPA and possibly other synthetic hormones on vascular health in young women.
Oral Contraceptive Use Linked to Small Increase in Cervical Cancer Risk November 16, 2007
The use of oral contraceptives is associated with an increase in the risk for invasive cervical cancer, researchers from the International Collaboration of Epidemiological Studies of Cervical Cancer report. An analysis of pooled data from 24 studies, published in the November 10 issue of The Lancet , found that for current users, the relative risk for cancer rises with increasing duration of oral contraceptive use.
Metabolism Volume 56, Issue 6, June 2007, Pages 830-837
Addition of medroxyprogesterone acetate to conjugated equine estrogens results in insulin resistance in adipose tissue
International Journal of Obesity (2004) 28, 998 -1003.
August 2004, Volume 28, Number 8, Pages 998-1003
Association between C-reactive protein, metabolic cardiovascular risk factors, obesity and oral contraceptive use in young adults
CONCLUSION: These findings suggest that obesity is associated with inflammation independent of other cardiovascular risk factors that may contribute to an increased risk for cardiovascular disease in men and women. Elevated CRP related to combined oral contraceptive use may influence the rate of cardiovascular events in young women.
Best Practice & Research Clinical Obstetrics & Gynaecology
Volume 17, Issue 3 , June 2003, Pages 509-528
Thrombophilias and gynaecology
In gynaecology, women are exposed to sex steroids when using oral contraceptives, hormone replacement therapy or when undergoing in vitro fertilization treatment and ovulation induction. Oral contraceptives and the use of hormone replacement therapy increase the risk of venous thrombosis.
Mutation Research/Genetic Toxicology and Environmental Mutagenesis
Volume 521, Issues 1-2 , 26 November 2002, Pages 113-119
Assessment of DNA damage in women using oral contraceptives
This study underscores the fact that prolonged and extensive use of these drugs in our daily life may be hazardous and also, that OC users should be aware of multifactorial risk factors (environmental, genetic and life style patterns) that may be responsible for additional DNA damage.
BJOG: An International Journal of Obstetrics and Gynaecology Volume 105 Issue 10 Page 1082 - October 1998
Norethisterone enanthate: the effect on postnatal depression and serum hormones
Conclusions Long-acting norethisterone enanthate given within 48 hours of delivery is associated with an increased risk of developing postnatal depression and causes suppression of endogenous ovarian hormone secretion.
BMJ 1999;318:96-100 ( 9 January )
Mortality associated with oral contraceptive use: 25 year follow up of cohort of 46 000 women from Royal College of General Practitioners' oral contraception study. Objective: To describe the long term effects of the use of oral contraceptives on mortality.
Pregnancy, Oral Contraceptives, Hormone Replacement Therapy As Risk Factors For Stroke
ScienceDaily (Apr. 16, 1997) - During the weeks immediately following delivery of a baby, new mothers are at increased risk of strokes, a University of Maryland School of Medicine neurology professor told the American Academy of Neurology meeting in Boston this week.
Journal of the National Cancer Institute 1995 87(11):827-835;
Oral Contraceptives and Breast Cancer Risk Among Younger Women. Among women younger than 45 years, oral contraceptive use for 6 months or longer was associated with an RR for breast cancer of 13 (95% CI = 1.1-1.5). Risks were enhanced for breast cancers occurring prior to age 35 years (RR = 1.7; 95% CI = 1.2-2.6), with the RR rising to 2.2 (95% CI = 1.2-4.1) for users of 10 or more years. The RR for breast cancer for those whose oral contraceptive use began early (before age 18 years) and continued long-term (>10 years) was even higher (RR = 3.1; 95% CI = 1.4-6.7). The RRs observed for those who used oral contraceptives within 5 years of cancer diagnosis were higher than for those who had not, with the effect most marked for women younger than age 35 years (RR = 2.0; 95% CI = 13-3.1). Oral contraceptive associations were also strongest for cancers diagnosed at advanced stages.
For more detail on contraceptives click here.
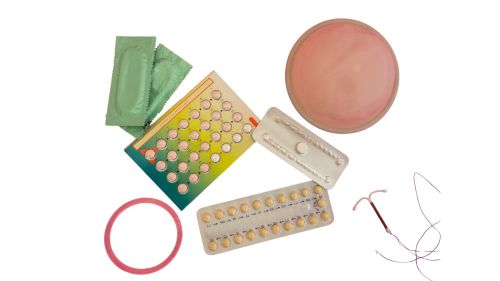 Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive…
Contraceptives are now ubiquitous, reaching even the most remote rural communities. But their widespread use raises an important question—at what cost to a woman’s health? All drug-based contraceptive… We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c…
We deeply value your trust and loyalty as part of the Natpro community. Over the past 30 years, we have worked hard to keep Natpro’s pricing stable, ensuring the highest quality natural progesterone c… Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea…
Hot flushes are the body’s attempt to regulate temperature, a natural response when it senses an imbalance. The skin, being the body’s main defence against overheating, responds with flushing and swea… Endometriosis is a perplexing and often distressing condition affecting an estimated one in five women during their reproductive years. It occurs when tissue similar to the endometrium — the lining of…
Endometriosis is a perplexing and often distressing condition affecting an estimated one in five women during their reproductive years. It occurs when tissue similar to the endometrium — the lining of…